Toxoplasmosis, caused by the parasite Toxoplasma gondii, is not a notifiable disease in most countries in Europe, so no real surveillance data are available.
WHO estimates there are over one million cases each year in the European region caused by contaminated food.
Challenging surveillance
Surveillance varies considerably between countries, posing a challenge in estimating the burden and outcomes of this disease, said the agency.
Healthy individuals infected with Toxoplasma gondii often do not develop symptoms because their immune system keeps the parasite from causing illness. Up to 95% of the population has been infected without developing symptoms.
When illness occurs, it is usually mild with “flu-like” symptoms that last for weeks to months. However, the parasite remains in the body in an inactive state and can become reactivated if the person becomes immunosuppressed.
Diagnosis of toxoplasmosis is typically made by serologic testing, which measures immunoglobulin G (IgG) titles to determine if a person has been infected.
Toxoplasma can be acquired trans-placentally (mother to baby), through contact with infected soil or water, ingestion of contaminated food or in very rare cases through blood/organ donation.
It is assumed that half the cases come from eating contaminated food, such as inadequately cooked animal meat or raw fruits and vegetables.
Prevention and trends
WHO said preventing foodborne toxoplasmosis involves effective hygiene including hand-washing and the use of clean water in food production and preparation is critical.
It added pregnant women should avoid undercooked meat and fruits and vegetables should be thoroughly washed with clean water.
Joke W. B. van der Giessen, epidemiologist at the National Institute for Public Health and the Environment (RIVM) Centre for Zoonoses and Environmental Microbiology in the Netherlands, said exposure might be declining in some areas of the EU due to changing animal husbandry practices.
“The decrease in seroprevalence is possibly linked to food animals being kept indoors, which decreases their exposure to Toxoplasma gondii oocysts via soil contamination,” she told WHO.
“In that case, transmission via meat of animals kept indoors might be lower. However, there are also other transmission routes to humans, such as fresh produce contaminated by oocysts shed by cats in the environment.”
Maria Vang Johansen, professor in parasitic zoonoses at the University of Copenhagen, Denmark, said trends are always evolving and changing, from food is raised to how it is prepared.
“There are no standard guidelines across Europe for how to prepare meat, and lowering the temperature in pork cooking guidelines in some countries poses a risk to consumers. Cooking meat until all potential pathogens have been eliminated is essential in preventing foodborne disease,” she told WHO.
“Zoonotic diseases cannot be fixed with one method alone: they need to be tackled through an integrated and one health (animal and human) approach. We must inform the public, secure our agriculture and food practices, conduct active and passive surveillance, and attack the parasite at many places in its life cycle.”
From 2003-2016, 1,091 patient samples were tested for T. gondii DNA by real-time PCR; 94 samples from 82 patients tested positive, according to the Laboratory of Parasitology at Statens Serum Institut (SSI) in Denmark.
Biological assays were previously used for direct detection of Toxoplasma, but the SSI now uses PCR, which is more sensitive, allows for standardisation and facilitates species-level identification.
Diagnosing toxoplasmosis is based mainly on antibody testing (indirect detection), whereas PCR may be used on suspicion of a specific focus.
It is being looked at if one or more T. gondii genotypes are associated with development of acute toxoplasmosis, said SSI.
Determining parasite presence
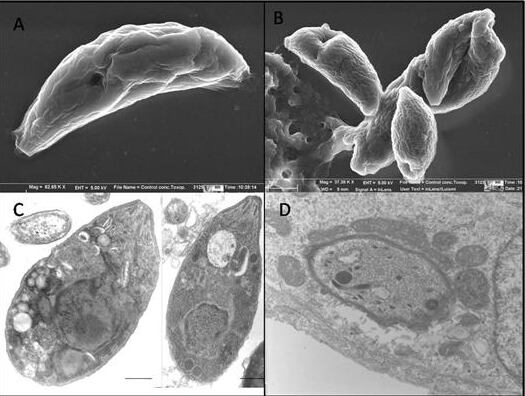
Meanwhile, scientists from the universities of Granada (UGR) and Valencia (UV) have developed a molecular method for determining the presence of the parasite in samples of ham.
It consists of capturing the parasite's DNA by magnetic particles functionalized with specific sequences of the parasite and quantification using a quantitative PCR (qPCR) technique.
The method is capable of detecting a parasite cell in 100g of ham sample with an efficiency of 94.6%.
They analyzed 475 commercial samples of ham in slices and cubes and estimated the number of T. gondii parasites present.
Results showed the prevalence of T. gondii in ham samples varied from 0% to 32.35%, depending on the production company.
The prevalence and viability of the parasite in ham samples depends on the production company and origin of the animals, which implies variations or noncompliance with regulations during the curing process, said the researchers.
They showed if ham meat samples are frozen before the curing process elimination of the parasite is much faster and the treatment normally used for curing ham using nitrites with sea salt increases Toxoplasma's survival time and infectivity rate, when compared to curing using only sea salt.
The freezing process is not covered by ham production regulations because it alters the organoleptic properties of some processed products.
The team suggested the traditional salting method for production of ham ensures total elimination of T. gondii, provided the curing period in the legislation is respected.
Use of nitrite during the salting process retards the inactivation of T. gondii, which makes higher curing periods (at least seven months) necessary to ensure complete elimination of the parasite.
